By the findings of mild lymphocytic pleocytosis and raised protein in CSF Thus, the main differentials considered were Lyme's disease, HIV, Kumar P, Charaniya R, Bahl A, Ghosh A, Dixit J Facial diplegia with paresthesia an uncommon variant of GuillainBarre syndrome J Clin Diagn Res 16;10(7)OD01–2 Neoplastic meningitis was also suspected but the patient's generalCerebrospinal fluid (CSF) protein level, cell count, and its relationship to the timing of lumbar puncture were collected from patients with GuillainBarré syndrome (GBS) and Miller Fisher syndrome (MFS) from various Asian centers A total of 507 patients with GBS were studied Overall, 56% had elevated CSF protein level This was significantly lower than that reported in a recentCerebrospinal fluid showed a raised protein concentration accompanied by mild pleocytosis Her symptoms resolved within two months Subsequent magnetic resonance imaging revealed cavity formation in the deep white matter and atrophic changes in the right occipital lobes GuillainBarré syndrome (GBS) is an acute demyelinating polyneuropathy presumably related to immuno
2
Guillain barre syndrome csf pleocytosis
Guillain barre syndrome csf pleocytosis- The relation between severe acute respiratory syndrome coronavirus 2 (SARSCoV2) infection and demyelinating GuillainBarre syndrome (GBS) has been defined We aim to report the clinical features of a child with axonal GBS associated with SARSCoV2 A 6yearold male presented with symmetric ascending paralysis progressed over a 4day course and 2 days ofIn cases with otherwise clinically typical Guillain–Barré syndrome (GBS), pronounced cerebrospinal fluid (CSF) pleocytosis or the mere presence of CSF‐polymorphonuclear granulocytes should alert the physician to consider alternative diagnoses Therefore, we retrospectively studied the neuropathology of central and peripheral nervous system in two cases with a CSF cell count of
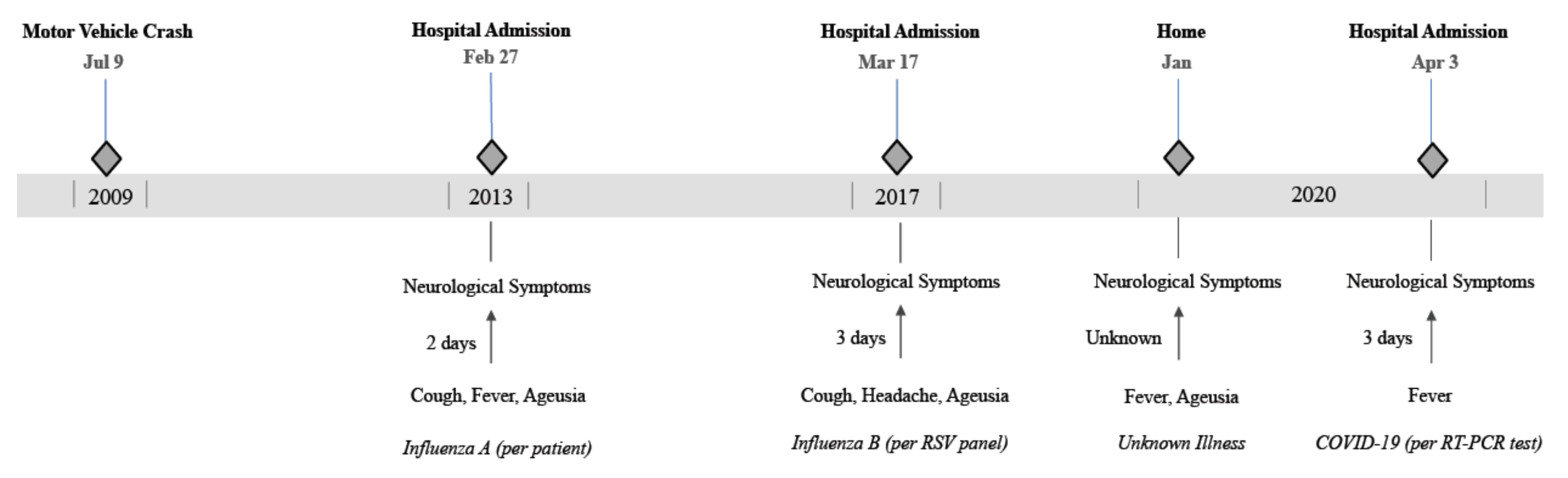



Pathogens Free Full Text Covid 19 As A Trigger Of Recurrent Guillain Barre Syndrome Html
The association of Guillain–Barré syndrome (GBS) with HIV infection has been noted soon after the beginning of the HIV infection epidemic The initial reports described it as typically occurring early in the course of HIV infection or even at the time of seroconversion Other than a commonly seen cerebrospinal fluid (CSF) pleocytosis, HIVassociated GBS (HIVGBS) is similarHowever, in this case, CSF analysis revealed an exaggerated pleocytosis (72 white blood cells (WBC)/mm 3) No source of central nervous system infection or inflammation was identified despite thorough investigation The patient was treated with intravenous immunoglobulin and intensive rehabilitationAlbuminocytological dissociation classically distinguishes GBS from infective CSF cell counts between 5 and 50 cells/μl, however, were found in 15% of patients, indicating that a mild pleocytosis is compatible with the diagnosis of GuillainBarré syndrome
1 Introduction Sarcoidosis is a multisystem granulomatous inflammatory disease Peripheral neuropathies occur in 15% of neurosarcoidosis patients 1 Mononeuritis multiplex is seen in 10% of patients with limb sarcoidosis neuropathy, 2 and neuropathies rarely present in a fashion similar to Guillain–Barré syndrome (GBS) We report, to our knowledge, the first patient with CSF pleocytosis is well recognized in HIVassociated GBS Previous Next Magnetic Resonance Imaging MRI is sensitive, but nonspecific, for diagnosis However, it can reveal nerve root enhancement and may be an effective diagnostic adjunct 111, 112 Spinal nerve root enhancement with gadolinium is a nonspecific feature seen in inflammatory conditions and isA systematic review from 1 January to 30 June revealed 42 patients with GuillainBarré syndrome (GBS) associated with SARSCoV2 infection Single cases and small series were reported from 13 countries, the majority from Europe (794%) and especially from Italy (309%) SARSCoV2 infection was demonstrated by nasopharyngeal swab (857%) and serology (143%)
Cerebrospinal fluid pleocytosis with neutrophil leukocytes in Guillain–Barré syndrome Berciano, J; In cases with otherwise clinically typical Guillain–Barré syndrome (GBS), pronounced cerebrospinal fluid (CSF) pleocytosis or the mere presence of CSF‐polymorphonuclear granulocytes should alert the physician to consider alternative diagnoses We could not test for SARSCoV2 in CSF in our case, but the absence of WBC in the CSF indicated an immune response typically seen in GBS rather than direct neuronal invasion, in which pleocytosis is expected MRI usually showed contrast enhancement of caudaequina nerve roots due to radicular irritation CSF showing CAD is usually observed in the second week after




Clinmed International Library Guillain Barre Syndrome With Lymphocytic Pleocytosis Of The Csf International Journal Of Brain Disorders And Treatment
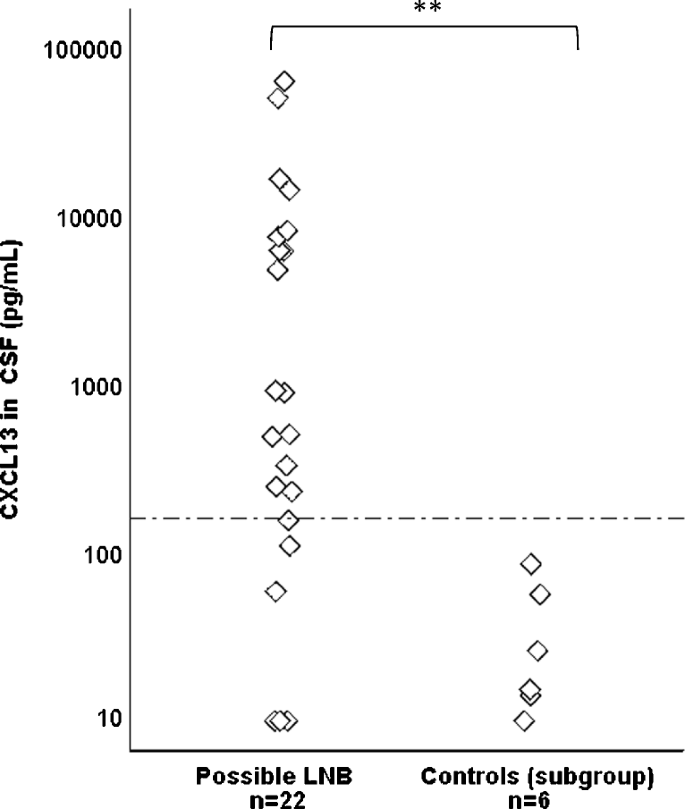



The Chemokine Cxcl13 In Cerebrospinal Fluid In Children With Lyme Neuroborreliosis Springerlink
GuillainBarre syndrome is an acute, inflammatory, postinfectious polyneuropathy A prodromal malaise with vomiting, headache, fever and limb pains is rapidly surmounted by a progressive and ascending paralysis This can lead to respiratory dysfunction, and as such, the acute presentation can be a neurological emergency GBS has an incidence of about 1/100,000 across severalGuillainBarre´ syndrome (GBS) is characterised by a classical triad of progressive motor weakness, areflexia and elevated cerebrospinal fluid (CSF) protein without pleocytosis1 Landry published the first modern description of an illness likely to be acute inflammatory demyelinating polyneuropathy (AIDP) in 1859 Osler provided a more Even if case of CSF pleocytosis (>50/ μ l) a differential diagnosis should be considered 1–2 this case report suggests that GuillainBarrè diagnosis can not defectively ruled out Previous article in issue




Guillain Barre Syndrome In The Elderly Experience From A Tertiary Care Hospital In India Journal Of Clinical Neuroscience



2
GuillainBarre´ Syndrome Ted M Burns, MD1 ABSTRACT GuillainBarre´ syndrome (GBS) is an acuteonset, monophasic, immunemediated polyneuropathy that often follows an antecedent infection The diagnosis relies heavily on the clinical impression obtained from the history and examination, although cerebrospinal fluid analysis and electrodiagnostic testing usually provideIn a followup study of 24 patients with GuillainBarre syndrome, 55% developed a cerebrospinal fluid (CSF) mononuclear pleocytosis, which persisted for 4 months or more Raised index values of CSFimmunoglobulin G (IgG), CSFIgA, and CSFIgM, indicating synthesis of the immunoglobulin in question in the central nervous system, were found in 63, 35, and 25%, respectively Agarose gelIn cases with otherwise clinically typical GuillainBarré syndrome (GBS), pronounced cerebrospinal fluid (CSF) pleocytosis or the mere presence of CSFpolymorphonuclear granulocytes should alert the physician to consider alternative diagnoses Therefore, we retrospectively studied the neuropathology of central and peripheral nervous system in two cases with a CSF cell count of




Guillain Barre Syndrome American Family Physician




What Is Guillain Barre Syndrome Mass4d Foot Orthotics
GuillainBarré syndrome is an acute autoimmune polyradiculoneuropathy with a clinical presentation of flaccid paralysis with areflexia, variable sensory disturbance, and elevated cerebrospinal fluid protein without pleocytosis Although GuillainBarré syndrome previously had been viewed as a unitary disorder with variations, it currently is viewed as a group of syndromes GuillainBarré syndrome has been reported in many countries and has a wide range of reported incidences ()1, 8 Populationbased studies from North America and Europe suggest that incidence ranges from 0·81 to 1·91 cases per 100 000 personyears (median 1·11)There is a % increase in incidence for every 10year increase in age, and unlike other autoimmune diseases, the risk of Guillain Background Diagnostic criteria for Guillain Barré syndrome (GBS) frequently require a pleocytosis of




Altered Mental Status In Guillain Barre Syndrome A Noteworthy Clinical Clue Mulroy Annals Of Clinical And Translational Neurology Wiley Online Library




Guillain Barre Syndrome Oncohema Key
Introduction GuillainBarre typically presents as a symmetric ascending weakness with areflexia The cerebrospinal fluid typically shows albuminocytologic dissociation In this case, we present an atypical presentation of severe GuillainBarre with cerebrospinal fluid exhibiting lymphocytic pleocytosis Case report 60yearold man presented with progressive lower extremityIn a followup study of 24 patients with GuillainBarré syndrome, 55% developed a cerebrospinal fluid (CSF) mononuclear pleocytosis, which persisted for 4 months or moreGuillainBarre syndrome (GBS) is an immunemediated polyneuropathy In the cerebrospinal fluid (CSF) characteristic increased protein without pleocytosis ie, albuminocytologic dissociation is seen But cases of GBS with significant CSF lymphocytosis have rarely been reported Here, we present a 38yearold man with dysarthria, dysphagia, bilateral facial palsy, and limb weakness




Temporal Profile Of Pain And Other Sensory Manifestations In Guillain Barre Syndrome During Ten Days Of Hospitalization Karkare K Taly Ab Sinha S Rao S Neurol India




Guillain Barre Syndrome Associated With Zika Virus Infection In Colombia Nejm
DOI // Authors Sneha Padidam Sneha Padidam This person is not on ResearchGate, or hasnGuillainBarré syndrome with exaggerated pleocytosis and antiGM1 ganglioside antibodies Gabriel Doctor, t CSF pleocytosis will have a high negative Table 1 Initial blood investigations value normal range Leucocytes (×109/L) 194 38–11 Lymphocytes (×109/L) 59 15–4 Neutrophils (×109/L) 119 2–75 CRP (mg/L) 41 CSF pleocytosis is well recognised in HIV associated GuillainBarré syndrome96 Electrophysiological features differ according to the clinicopathological type (box 3)15, 68, 95 Magnetic resonance imaging can be useful in diagnosis, especially when the electrophysiological findings are equivocal




Guillain Barre Syndrome
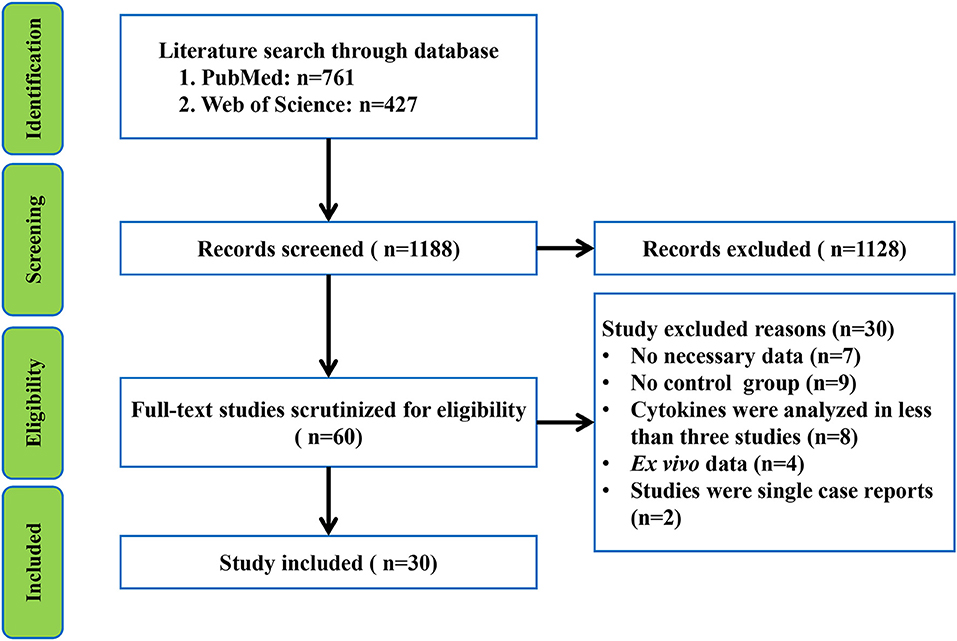



Frontiers Peripheral Blood And Cerebrospinal Fluid Cytokine Levels In Guillain Barre Syndrome A Systematic Review And Meta Analysis Neuroscience
Guillain Barre syndrome is an elevated CSF protein content without a pleocytosis 6,7 The most typical neuroimmunological response in pa tients with Guillain Barre syndrome is the blood barrier dysfunction, it can be valued easily with the reibergram or CSF/serum quotient graphs 1,2 There are diagrams that analyze in an integrated way both the function of the bloodCSF barrierGuillainBarré syndrome, bifacial weakness with paraesthesias, headache, pleocytosis, plasma exchange CASE DESCRIPTION A 50yearold woman, with no significant medical history, presented to the emergency department with a 10day history of severe, bilateral, occipital headache and inability to close the lips and both eyesCerebrospinal fluid (CSF) with a total protein of 45 mg% and an increased IgG fraction (15%) CSF glucose was normal, and there was no pleocytosis CSF cultures were sterile AAEE Case Report #4 GuillainBarr6 Syndrome MUSCLE & NERVE September 19 705




Guillain Barre Syndrome And Other Immune Mediated Neuropathies Diseases Of The Nervous System Harrison S Neurology In Clinical Medicine 3rd Edition



Abstract Guillain Barre Syndrome Gbs Is Generally Considered To Be Monophasic But Recurrences Do Occur In Some Patients We Report A Case Of A 57 Year Old Male Hypertensive Euglycaemic With Prior History Of Gbs 7 Years Ago Presented With
Lafarga, M Dear Sir, We read with interest the paper by Rauschka (03) concerning the clinico‐pathological study of five cases of Guillain–Barré syndrome (GBS) whose cerebrospinal fluid (CSF) examinations showed pronounced pleocytosis Introduction GuillainBarré syndrome (GBS) is the most common cause of acute flaccid paralysis in childhood with an incidence of about 08 per 100,000 children under 15 years of age per annum ()It is an acute inflammatory polyneuropathy, characterized by rapidly progressive, symmetrical flaccid paralysis and areflexia ()Weakness is more often initially distally Guillain–Barré syndrome (GBS) is the most frequent cause of subacute neuromuscular weakness in North America The median incidence of GBS is about 1 per 100 000 personyears, with higher rates in older people (a % increase in the average GBS rate for every 10year increase in age) and males1 Infections can trigger GBS (eg, including those caused by Campylobacter




Guillain Barre Syndrome




Guillain Barre Syndrome Mayo Clinic Proceedings
Rauschka H, Jellinger K, Lassmann H, Braier F, Schmidbauer M GuillainBarré syndrome with marked pleocytosis or a significant proportion of polymorphonuclear granulocytes in the cerebrospinal fluid neuropathological investigation of five cases and review of differential diagnoses Eur J Neurol 03 Sep;10(5)479–86 In healthcare settings where there is a low prior probability of an infectious cause of flaccid paralysis, cerebrospinal fluid pleocytosis should not exclude a diagnosis of GBS and antiganglioside antibody testing can be particularly helpful References ↵ Guillain G, Barré JA, Strohl A Sur un syndrome de radiculonévrite avec hyperalbuminose du liquide céphalorachidien sans GuillainBarre syndrome (GBS) is the most common cause of acute, flaccid, neuromuscular paralysis in the United States GuillainBarre syndrome was first discovered more than a century ago Advances in the past century include investigating the immunemediated pathophysiology of the disease, recognizing the spectrum of presentations, advancing diagnostic




Age Matters Neurology Neuroimmunology Neuroinflammation




300 Usmle Rx Bricks Neurology Ideas In 21 Neurology Medical Education Nursing Notes
Cerebrospinal fluid showed a raised protein concentration accompanied by mild pleocytosis Her symptoms resolved within two months Subsequent magnetic resonance imaging revealed cavity formation in the deep white matter and atrophic changes in the right occipital lobes We report the clinical course, and neurophysiological and neuroimaging findings of a patient with GuillainBarré syndrome GuillainBarré Syndrome Following Chickenpox With Multiple Cranial Nerve Palsies and Cerebrospinal Fluid Pleocytosis AntiGM1 and Campylobacter serology were both positive, consistent with postinfectious axonalvariant GuillainBarré syndrome (GBS) GBS is characterised by albuminocytological dissociation, where an elevated protein and acellular cerebrospinal fluid are typical However, in this case, CSF analysis revealed an exaggerated pleocytosis (72 white




Cerebrospinal Fluid Findings In Neurological Diseases Associated With Covid 19 And Insights Into Mechanisms Of Disease Development International Journal Of Infectious Diseases
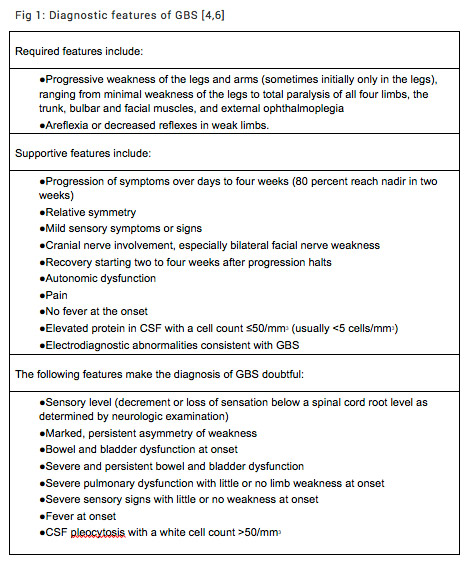



Guillain Barre Syndrome Rcemlearning
In a followup study of 24 patients with GuillainBarré syndrome, 55% developed a cerebrospinal fluid (CSF) mononuclear pleocytosis, which persisted for 4 months or more Raised index values of CSFimmunoglobulin G (IgG), CSFIgA, and CSFIgM, indicating synthesis of the immunoglobulin in question in the central nervous system, were found in 63, 35, and 25%, respectively Agarose gelGuillainBarre Syndrome with Lymphocytic Pleocytosis of the CSF December 15; GuillainBarré syndrome (GBS) is a rare complication of chickenpox All cases of postvaricella GBS published in the literature have been associated with the classical albuminocytological dissociation We report the case of a 48yearold male with flaccid areflexic quadriparesis and bilateral seventh, ninth, tenth, and twelfth cranial nerve palsies 10 days after



3




Guillain Barre Syndrome The Lancet




Scielo Brasil Oligosymptomatic Dengue Infection A Potential Cause Of Guillain Barre Syndrome Oligosymptomatic Dengue Infection A Potential Cause Of Guillain Barre Syndrome




Diagnosis Of Guillain Barre Syndrome In Children And Validation Of The Brighton Criteria Topic Of Research Paper In Clinical Medicine Download Scholarly Article Pdf And Read For Free On Cyberleninka Open Science




Clinical Variants Of Guillain Barre Syndrome In Children Pediatric Neurology




Pdf Guillain Barre Syndrome Following Chickenpox With Multiple Cranial Nerve Palsies And Cerebrospinal Fluid Pleocytosis
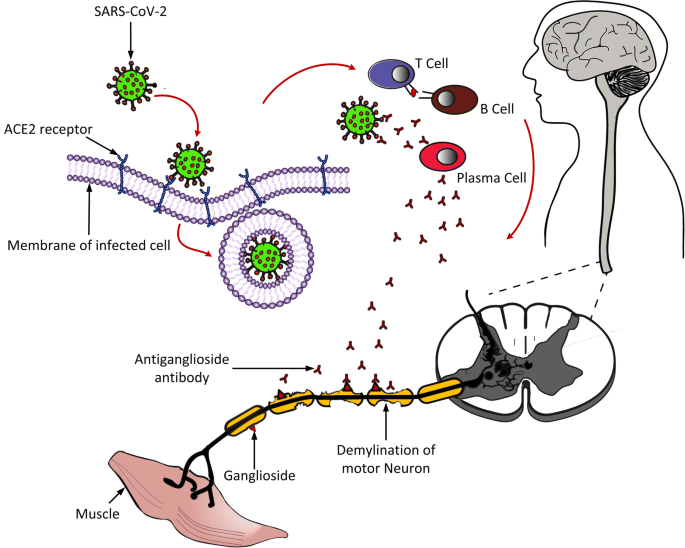



Covid 19 Associated Guillain Barre Syndrome Atypical Para Infectious Profile Symptom Overlap And Increased Risk Of Severe Neurological Complications Springerlink




Pdf Diagnosis Of Guillain Barre Syndrome And Validation Of Brighton Criteria Semantic Scholar




Pdf Guillain Barre Syndrome Semantic Scholar




Guillain Barre Syndrome Variant Occurring After Sars Cov 2 Vaccination Allen 21 Annals Of Neurology Wiley Online Library




Comparison Of Tm And Gbs Download Table




Csf Neurofilament Levels A Potential Prognostic Marker In Guillain Barre Syndrome Semantic Scholar
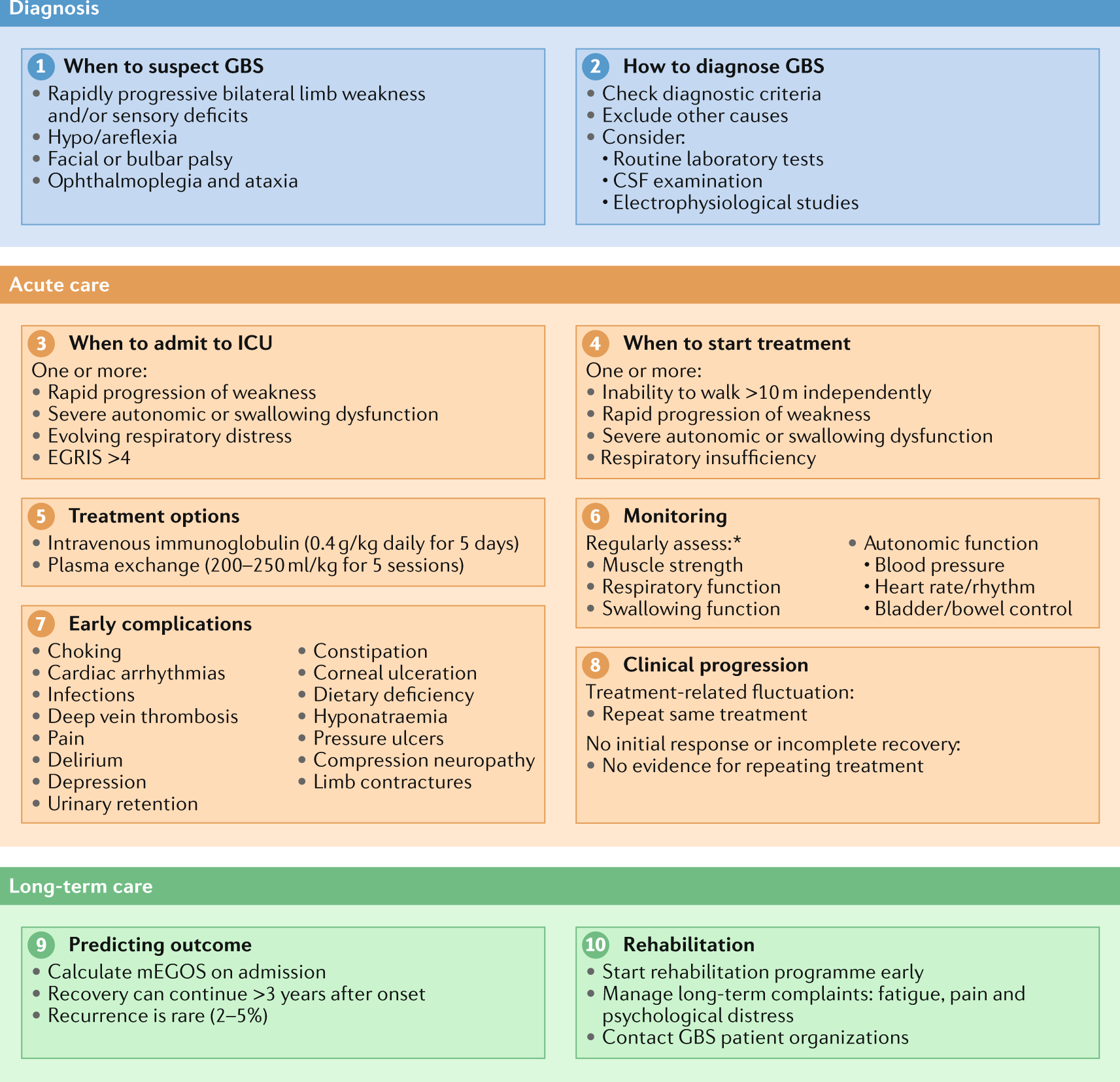




Diagnosis And Management Of Guillain Barre Syndrome In Ten Steps Nature Reviews Neurology



1



3
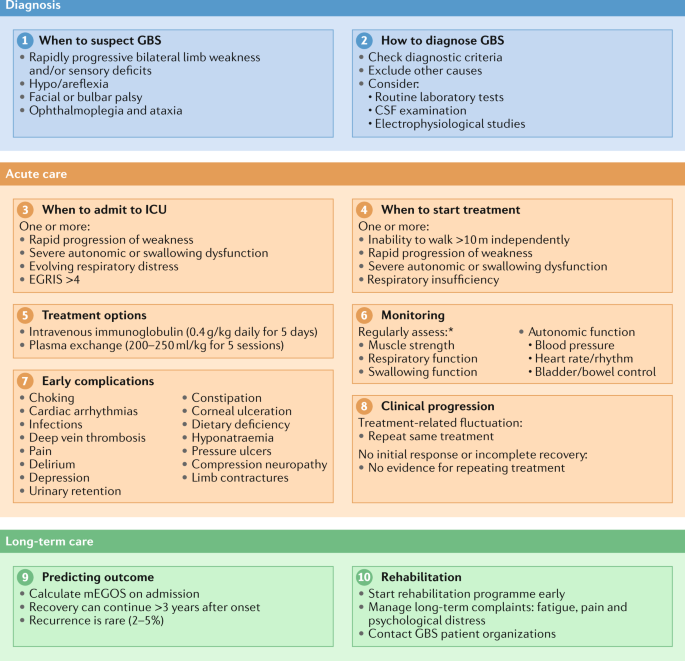




Diagnosis And Management Of Guillain Barre Syndrome In Ten Steps Nature Reviews Neurology



2




Guillain Barre Syndrome In Taiwan A Clinical Study Of 167 Patients Journal Of Neurology Neurosurgery Psychiatry




Guillain Barre Syndrome Mimics Tham 18 Brain And Behavior Wiley Online Library




Guillain Barre Syndrome




The Management Of Guillain Barre Syndrome Current Paediatrics




Guillain Barre Syndrome Nejm




8 Guillain Barre Syndrome Ideas Guillain Barre Syndrome Barre Syndrome



Criteria Blood Gov Au




Igm In Serum And Csf Of Gbs Patients Download Table




Cerebrospinal Fluid In Covid 19 A Systematic Review Of The Literature Sciencedirect



Revistanefrologia Com
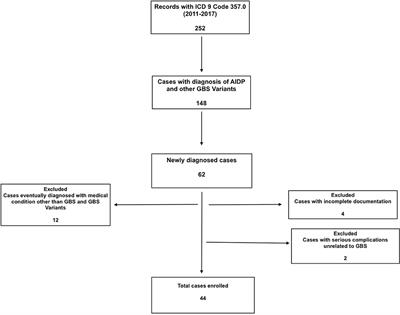



Cerebrospinal Fluid Analysis List Of Frontiers Open Access Articles




Guillain Barre Syndrome In Taiwan A Clinical Study Of 167 Patients Journal Of Neurology Neurosurgery Psychiatry



1




Scielo Brasil Assessment Of Acute Motor Deficit In The Pediatric Emergency Room Assessment Of Acute Motor Deficit In The Pediatric Emergency Room




Clinical Significance Of Serum And Csf Findings In The Guillain Barre Syndrome And Related Disorders Semantic Scholar




Findings Of Cerebrospinal Fluid During The Initial Presentation In 02 Download Scientific Diagram




Guillain Barre Syndrome Pdf Nerve Neurological Disorders




The Guillain Barre Syndrome Report Of A Case Treated With Acth And Cortisone Nejm



2




Guillain Barre Syndrome




25 Neurodegenerative Ideas Nursing Study Nursing Notes Nursing Mnemonics




Guillain Barre Syndrome Neupsy Key



2




Laboratory Findings At Initial Presentation And Recurrence Of Download Table




Comparison Of Intravenous Immunoglobulin And Plasma Exchange In Treatment Of Mechanically Ventilated Children With Guillain Barre Syndrome A Randomized Study Topic Of Research Paper In Clinical Medicine Download Scholarly Article Pdf




Clinical Significance Of Serum And Csf Findings In The Guillain Barre Syndrome And Related Disorders Semantic Scholar




Lymphocytic Pleocytosis Wikipedia




Guillain Barre Syndrome American Academy Of Pediatrics




Guillain Barre Syndrome Ppt Video Online Download




Scielo Brasil Acute Inflammatory Demyelinating Polyradiculoneuropathy Guillain Barre Syndrome Following Dengue Fever Acute Inflammatory Demyelinating Polyradiculoneuropathy Guillain Barre Syndrome Following Dengue Fever




Clinical Features And Prognosis With Guillain Barre Syndrome




Poliomyelitis Poliomyelitis Is A Clinicopathologic Syndrome Characterized By




Guillain Barre Syndrome
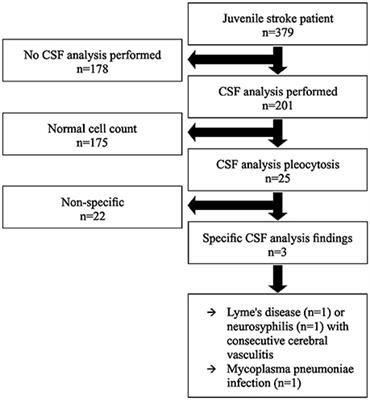



Cerebrospinal Fluid Analysis List Of Frontiers Open Access Articles




Guillain Barre Syndrome The Lancet




Jaypeedigital Ebook Reader




Program Information Ppt Download




Guillain Barre Syndrome American Family Physician




Pathogens Free Full Text Covid 19 As A Trigger Of Recurrent Guillain Barre Syndrome Html



2




Jkms Journal Of Korean Medical Science



Improved A Guillain Barre Syndrome Patient With Positive Pcr Test For Coronavirus In Cerebrospinal Fluid After Plasmapheresis A Case Report Jentashapir Journal Of Cellular And Molecular Biology Full Text




Pdf Pleocytosis And Immunoglobulin Changes In Cerebrospinal Fluid And Herpesvirus Serology In Patients With Guillain Barre Syndrome




Guillain Barre Syndrome American Family Physician



709 Ancillary Tests For Gbs Csf Findings Classic Precedent Infection Mangement How Can The Respiratory Status Of A Gbs Patient Be Easily Followed Emupdates




Pdf Guillain Barre Syndrome Presenting With Severe Hydrocephalus In A Child



2
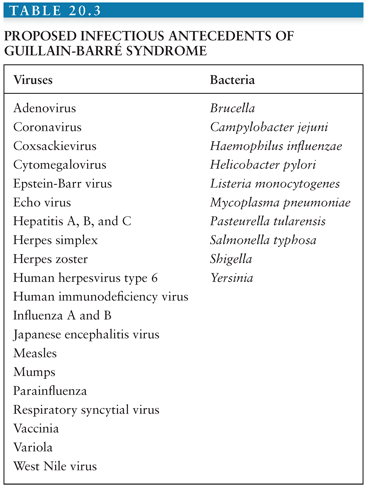



Guillain Barre Syndrome Oncohema Key




Guillain Barre Syndrome Ppt Download




Guillain Barre Syndrome And Other Immune Mediated Neuropathies Diseases Of The Nervous System Harrison S Neurology In Clinical Medicine 3rd Edition
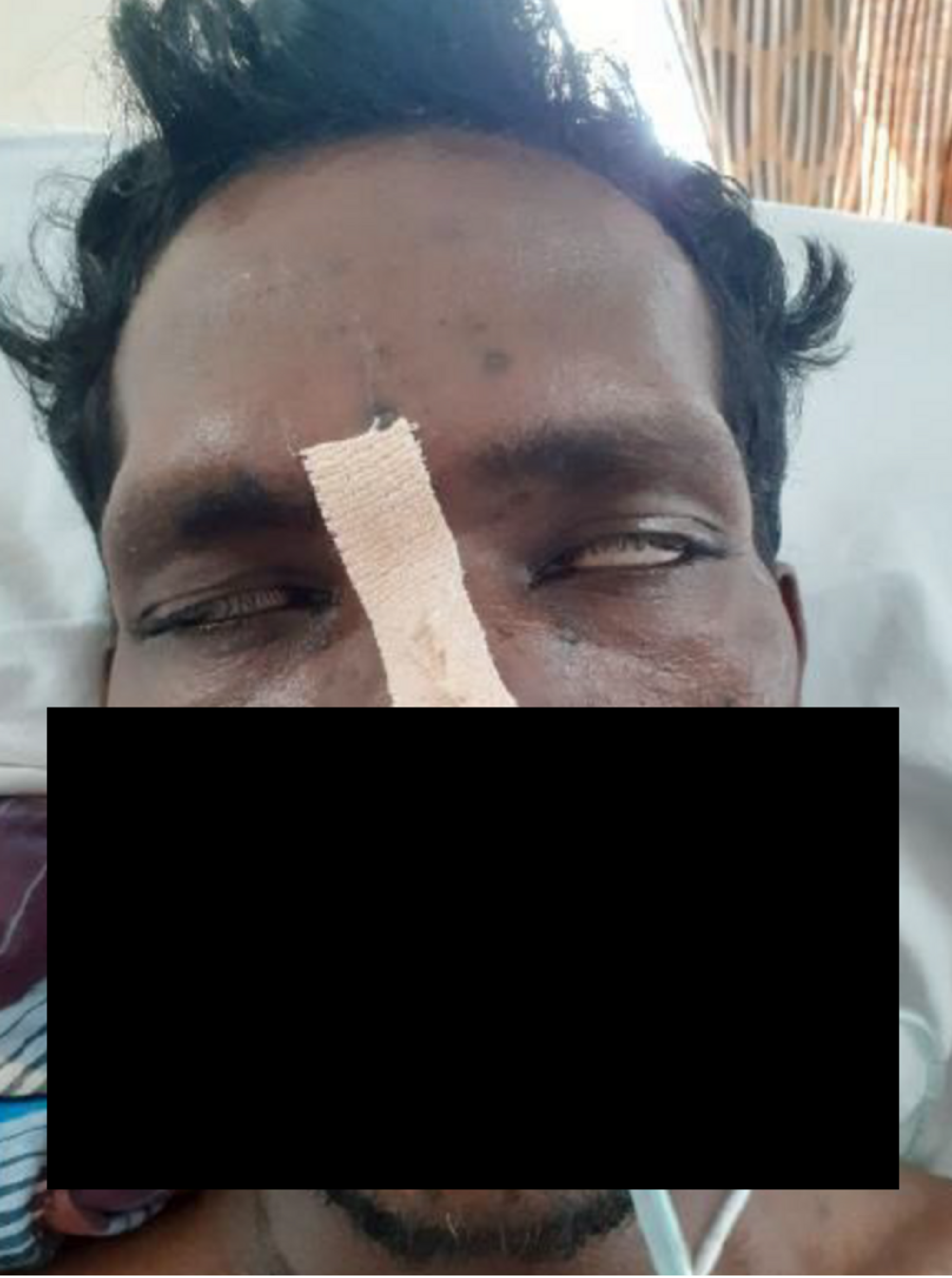



Cureus Guillain Barre Syndrome Following Chickenpox With Multiple Cranial Nerve Palsies And Cerebrospinal Fluid Pleocytosis
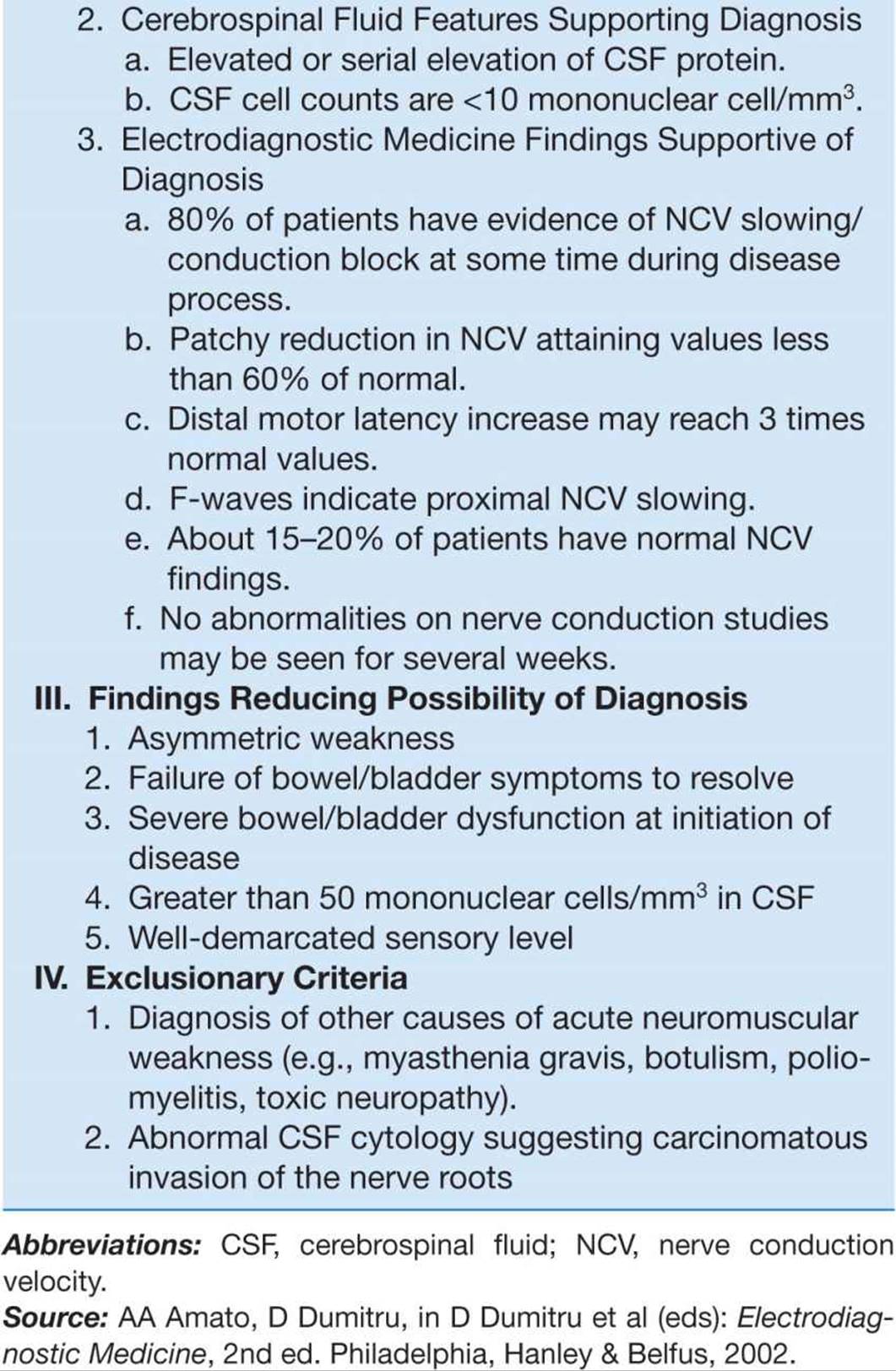



Guillain Barre Syndrome And Other Immune Mediated Neuropathies Diseases Of The Nervous System Harrison S Neurology In Clinical Medicine 3rd Edition



2




Guillain Barre Syndrome The Lancet




Causes Of Albuminocytological Dissociation And The Impact Of Age Adjusted Cerebrospinal Fluid Protein Reference Intervals A Retrospective Chart Review Of 2627 Samples Collected At Tertiary Care Centre Bmj Open




Age Matters Neurology Neuroimmunology Neuroinflammation




Csf Filtration Is An Effective Treatment Of Guillain Barre Syndrome Neurology
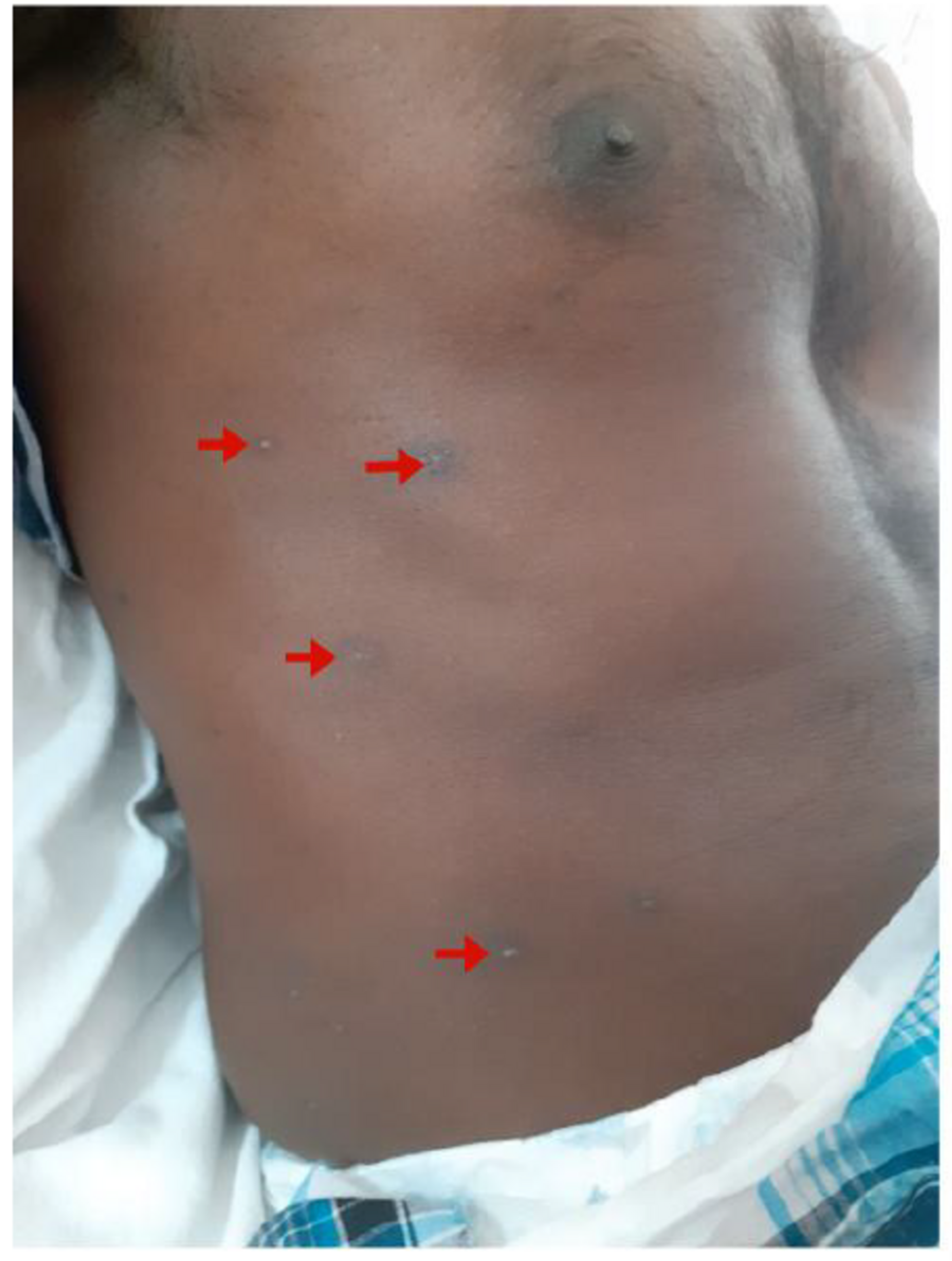



Cureus Guillain Barre Syndrome Following Chickenpox With Multiple Cranial Nerve Palsies And Cerebrospinal Fluid Pleocytosis




Beyond Lnb Real Life Data On Occurrence And Extent Of Csf Cxcl13 In Neuroinflammatory Diseases Journal Of Neuroimmunology




The Guillain Barre Syndrome Nejm



Exam Questions Cicm 18 2 3




Gbs 2 Pdf Myelin Meningitis



Abstract Guillain Barre Syndrome Gbs Is Generally Considered To Be Monophasic But Recurrences Do Occur In Some Patients We Report A Case Of A 57 Year Old Male Hypertensive Euglycaemic With Prior History Of Gbs 7 Years Ago Presented With




A 69 Year Old Woman With Double Vision And Lower Extremity Weakness Consult Qd




Csf Findings In Guillain Barre Syndrome Demyelinating And Axonal Acute Inflammatory Polyneuropathies Springerlink




Clinical Features And Prognosis With Guillain Barre Syndrome Topic Of Research Paper In Clinical Medicine Download Scholarly Article Pdf And Read For Free On Cyberleninka Open Science Hub
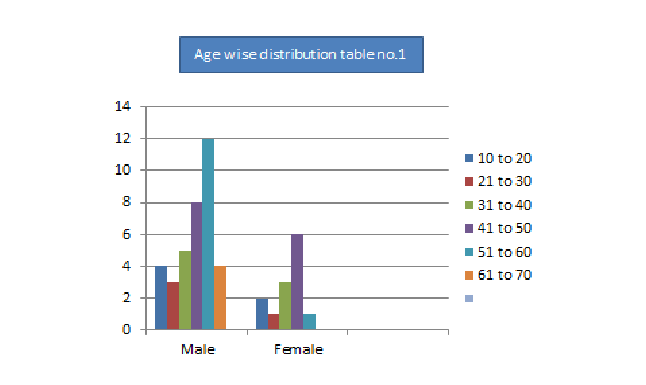



Guillain Barre Syndrome Clinical Profile Journal Of Current Medical Research And Opinion



0 件のコメント:
コメントを投稿